Last update: 11 July 2023
Introduction
An example of patient’s own experience of being used as an interface between sponsors and participants of clinical trials. Taking place both in rare diseases with EURORDIS and HIV / AIDS Act Up, Traitements & Recherche Thérapeutique (TRT-5) and the European AIDS Treatment group (EATG).
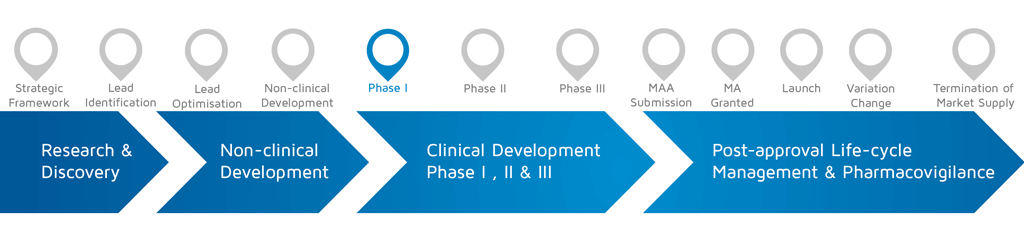
- When does it happen? – Phase I
Description of the case
The numbers of clinical trials in the design, conduct, DSMB, results analysis and communication of which the patient advocate was personally involved approximates 77. This includes trials with a few hundreds to a few thousand patients.
Methods:
- TRT-5: SOP approved by the national AIDS research agency (ANRS) according to which all protocols of clinical trials in AIDS/HIV (including opportunistic diseases), viral hepatitis and other viral diseases have to be discussed with patients’ advocates prior to their submission to ethics committee, and progress review for each of them all along the clinical trials.
- In parallel TRT-5 also met with private sponsors (industry) but on a voluntary basis.
- EATG/European Community Advisory Board: from 1996 to 2002, on a voluntary basis, clinical trials run by industry or public research organisations (e.g. INITIO trial by HIV Connect).
- EURORDIS: Implementation of the Charter for Clinical Trials in Rare Diseases signed by seven companies, one of which has signed a memorandum of understanding with relevant patients’ organisations (working together on two clinical trials and one compassionate use programme).
Type(s) of patient (advocates) involved
- Patients with personal disease experience.
- Expert patients / patient advocates with good expertise on disease, but little R&D experience.
- Expert patients / patient advocates with good expertise on disease and good R&D experience.
- Patient advocates with no expertise on the disease and good R&D experience.
Benefits of patient involvement
No systematic evaluation of the processes and results in the methods explained above.
However this whole process made possible:
- Substantial changes in CT protocols: Discussion on the therapeutic index led a sponsor to add one arm to a Phase III trial testing a dose that wasn’t initially proposed by the investigators. This dose turned out to be the authorised dose when was authorised.
- Substantial changes in the product development plan: Trials which had not been planned by the company but proposed by advocates were added and successfully conducted.
- Interruption of trials: Trials which had been authorised and approved by ethics committees were finally interrupted as patient advocates expressed ethical issues after the trial had started.
- Choice of the relevant outcome: For rare diseases, when no or little clinical research has been conducted before, it is essential to listen to patients for the identification / adaptation / creation of a relevant outcome.
Challenges and barriers
- Table of decisions and follow-up: It is essential to keep track of all discussions, text modifications and proposals made -a good secretariat managed by the patients.
- Confidentiality undertaking: Signed documents are essential. If no confidentiality documents signed, don’t even meet with sponsor, this is waste of time.
- Insider trading: Ensure this risk is reduced, have participants sign an agreement not to use the information to buy or sell shares on the stock exchange.
- Consistency of the opinion given: Ensure long term commitment of patients’ advocates and a pool of volunteers / staff with a good communication between all (see also first point above).
- Conflicts of interest prevention: Transparency, share the agenda / minutes of the meeting with regulatory authorities.
- Transparency with the patients’ community at large: Define what will be discussed, agree what will be confidential and what won’t be.
- Adequate training / mentorship.
Learnings
Whom to interact with exactly? For public sponsors usually the main investigator. Private sponsors can mean (1) public relations and marketing department, (2) research team, (3) a mix. Only (2) should be considered.
How to make sure decision makers interact with the advocates? And not simply go-between with little if no capacity to influence the sponsor’s senior management?
For international trials, how to coordinate with advocates across the world?
Head-to-head comparisons ort multifactorial design trials where cooperation between competitors is needed: this is typically not happening, and yet very much needed. How to improve this?
Dialogue on R&D is not just about obtaining marketing authorisation and/or reimbursement. How to open dialogue on the company’s corporate responsibility at large?
CT results and how to inform the trials’ participants at the same time than investigators.
A3-sponsors-participants-V1
Attachments
- Patients Involved Case Report – Between Sponsors and Participants of a clinical trial
Size: 458,234 bytes, Format: .pdf
An infographic describing a patients involved case report of a patient advocate acting as an interface between sponsors and participants of a clinical trial in the field of HIV and rare diseases.